What is Immunophenotyping?
Immunophenotyping is a technique that utilizes specific antibodies to target and identify unique surface markers or antigens expressed on immune cells, providing a detailed characterization of these cell populations. CD (cluster of differentiation) antibodies, which bind specific cell surface antigens and follow a standardized nomenclature, are commonly used for this purpose. The fluorescence emitted by labeled antibodies can be measured by flow cytometry (FC) and fluorescence-activated cell sorting (FACS™), enabling rapid and simultaneous analysis of multiple cellular parameters.
A newer technique called mass cytometry or CyTOF® (cytometry by time-of-flight) employs metal isotopes as labels and allows robust analysis of up to 60 individual parameters simultaneously (see Cossarizza et al. 2019 for a comprehensive review of methods). Simultaneous measurements with multiple antibodies offer enhanced specificity and sensitivity, facilitating comprehensive and precise characterization of complex cell populations.
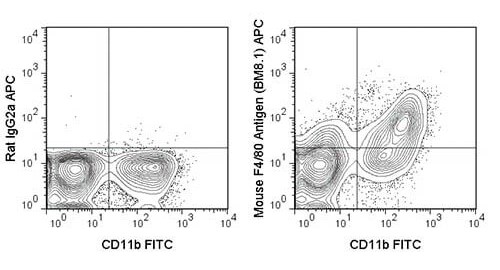
Flow cytometry analysis of C57BL/6 bone marrow cells with isotype control (left) and F4/80 APC Conjugated Monoclonal Antibody (right).
Features and Benefits of Immunophenotyping
Accurate Immune Cell Identification
Immunophenotyping enables precise identification and quantification of immune cells, offering a comprehensive understanding of the immune system. By utilizing antibodies specific to surface markers on immune cells (e.g. CD markers), flow cytometry analysis allows researchers to discern distinct immune cell populations.Biomarker Discovery
Immunophenotyping plays a pivotal role in biomarker discovery, revolutionizing diagnostic and prognostic approaches. By evaluating the expression patterns of surface markers on immune cells, researchers can identify novel biomarkers that provide valuable insights into disease progression, treatment response, and personalized medicine.Disease Characterization
Immunophenotyping serves as a diagnostic tool for disease characterization. By analyzing immune cell subsets and their unique surface markers, researchers gain insights into immune dysregulation, immune-mediated disorders, and the effectiveness of therapeutic interventions. This knowledge paves the way for tailored treatment strategies and improved patient outcomes.Immune Profiling
Immunophenotyping offers a comprehensive immune profile, facilitating a deeper understanding of immune responses. By evaluating immune cell populations and their phenotypic characteristics, researchers can unravel the complexities of immune regulation, immunodeficiencies, and immune-related disorders.Immunophenotyping, powered by flow cytometry and targeted antibodies, has revolutionized cellular analysis in immunological studies. With its ability to identify immune cell subsets, discover biomarkers, and characterize diseases, immunophenotyping offers a comprehensive view of the immune system.
Rockland Flow Cytometry Antibodies
CD Markers for Immunophenotyping
| Cell Type | Human | Mouse |
| B Cells | CD19, CD20 | CD19, CD20 |
| Cytotoxic T Cells | CD8 | CD8 |
| Dendritic Cells | CD11c | CD11c |
| Endothelial Cells | CD146 | CD146 |
| Epithelial Cells | CD326 | CD326 |
| Erythrocyte | CD235a | CD235a |
| Granulocytes | CD66b | Ly6G |
| Hematopoetic Stem Cells | CD34 | CD34 |
| Leukocytes | CD45 | CD45 |
| Monocytes / Macrophages | CD14, CD33 | CD11b, F4/80 |
| Natural Killer Cells | CD56 | CD335 |
| Platelets | CD41, CD61 | CD41, CD61 |
| T Cells | CD3 | CD3 |
| T Helper Cells | CD4 | CD4 |
Flow Cytometry Markers in Disease
| Disease | Suitable Surface Markers |
| Acute Myeloid Leukemia (AML) | CD2, CD3, CD4, CD5, CD7, CD8, CD10, CD13, CD14, CD15, CD16, CD19, CD20, CD30, CD33, CD34, CD38, CD45, CD56, CD64, CD71, CD117, CD123, HLA-DR |
| Adult T-Cell Leukemia/Lymphoma | CD7, CD25, HTLV-1 |
| Autoimmune Lymphoproliferative Syndrome (ALPS) | CD4, CD8, TCRα, TCRβ |
| Automosomal Recessive Hyper-IgM (HIGM) | CD40 |
| Burkitt Lymphoma | BCL-2, CD10 (+b), CD43 |
| Chronic Lymphocytic Leukemia | CD20, CD22, CD23, FMC-7 |
| Common Variable Immunodeficiency | CD21, CD40L |
| CTLA4 Haploinsufficiency | CTLA4 |
| Diffuse Large B-Cell Lymphoma | BCL-2, CD43 |
| DOCK8 Deficiency | DOCK8 |
| Eosinophilic Otitis Media | Eosinophils |
| Familial Hemophagocytic Lymphohistiocytosis | Perforin |
| Follicular Lymphoma | BCL-2, CD43 |
| Hairy Cell Leukemia | CD11c, CD20, CD22, CD25, CD103, sIg (I) |
| Immune Dysregulation (IPEX) | Foxp3 |
| IRAK4 and UNC93B Deficiency | CD62L |
| Leukocyte Adhesion Deficiency (LAD) Type 1 | CD11b, CD11c, CD18 |
| Leukocyte Adhesion Deficiency (LAD) Type 2 | CD15s |
| LRBA Deficiency | CTLA4, LRBA |
| Mantle Cell Lymphoma | CD5, CD20 |
| MHC Class II Deficiency | HLA-DR |
| Multiple Myeloma | Plasma Cells |
| Non-Small Cell Lung Cancer (NSCLC) | PDL1 (CD274) |
| Prolymphocytic Leukemia | CD5, CD20 (+i), sIg (+i), FMC-7 |
| T-Cell Large Granular Lymphocyte Leukemia | CD5, CD7, CD16, CD56, granzyme-B, perforin |
| X-Linked Hyper-IgM (HIGM) | CD40L |
| X-Linked Agammaglobulinemia (XLA) | BTK |
| X-Linked Lymphoproliferative Syndrome (XLP1/2) | SAP, XIAP |
Table adapted from Herold & Mitra 2022 and Delmonte & Fleischer 2018
References
- Cossarizza, A., Chang, H. D., Radbruch, A., Acs, A., Adam, D., Adam-Klages, S., Agace, W. W., Aghaeepour, N., Akdis, M., Allez, M., Almeida, L. N., Alvisi, G., Anderson, G., Andrä, I., Annunziato, F., Anselmo, A., Bacher, P., Baldari, C. T., Bari, S., Barnaba, V., … Zychlinsky, A. (2019). Guidelines for the use of flow cytometry and cell sorting in immunological studies (second edition). European journal of immunology, 49(10), 1457–1973.
- Herold NC, Mitra P. Immunophenotyping. [Updated 2022 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Delmonte, O. M., & Fleisher, T. A. (2019). Flow cytometry: Surface markers and beyond. The Journal of allergy and clinical immunology, 143(2), 528–537.