The Utility of Antibodies When Investigating SARS-CoV-2 and Variants of Concern
In late 2019, the world was confronted by a health crisis that few had foreseen. If you studied pandemics throughout history, you knew the next emergence and spread of an infectious disease was inevitable, but few people or governments were prepared for how the disease would afflict humanity. By early 2020, the SARS-CoV-2 coronavirus—first identified in Wuhan, China— spread across the globe. In a matter of months, the highly transmissible respiratory infection, COVID-19, could be found in six continents.
Coronaviruses are known to cause respiratory tract infections in mammals and birds, along with additional illnesses in other animals. And while some coronaviruses cause routine illnesses that most people have experienced at least once in their lives, other more lethal types can cause severe illness or death, although less common.
Common coronaviruses affecting humans with designations, such as 229E, NL63, OC43, and HKU1, usually cause mild to moderate upper-respiratory tract illnesses like the common cold. But uncommon coronaviruses can be deadly, such as the virus that caused an outbreak in 2002 of Severe Acute Respiratory Syndrome (SARS), inflicting over 8000 people, or the outbreak of Middle East Respiratory Syndrome (MERS) in 2012. These uncommon coronaviruses have variable rates of infectivity, transmissibility, hospitalization, and mortality and the longer the virus persists in human populations, the more likely the virus is to mutate in an effort by the virus to remain viable and propagate within the pool of susceptible hosts.
Vaccination and acquired immunity add additional pressure on the virus to alter its genetic sequence, especially within the most immunogenic regions of the virus, which can coincide with the epitope for vaccination and result in immunoevasion. If the virus can persist globally in areas with high populations of immunocompromised individuals, then the formula for viral mutation can become explosive.
Variants
The first SARS-CoV-2 infection in the United States was identified in January 2020 in Washington state. It quickly spread and was subsequently isolated and sequenced from these initial infections; this information served as a reference as the public health community tracked the outbreak. The high transmissibility of SARS-CoV-2 led to the first detection of a SARS-CoV-2 variant in late 2020 in the United Kingdom. Over a year later, no less than 13 other variants and subvariants have been identified.1 One of the latest variants, Omicron, has been identified by the Centers for Disease Control and Prevention as a Variant of Concern (VOC).
Unlike some other variants, Omicron, which was first isolated in Southern Africa, was found to have over 50 mutations relative to the canonical sequence. The Omicron variant has the distinction of having at least 22 novel mutations to the Spike protein (S) gene alone, including 14 mutations shared by other variants.2 The Spike protein is known to be the point of cell infection for the virus; therefore, it has been the focus of antibody development for diagnostics and therapeutics and coincides with many points of mutations in VOC.
Drawbacks of Monoclonal Antibodies
The number of mutations and their locations on the S protein has been shown to be problematic for current public safety procedures. The diagnostic industry has heavily relied on monoclonal antibodies for use as critical reagents in immunoassays. Their unique attributes allow for lot-to-lot consistency, rapid upscaling, and affordability. Many COVID-19 rapid antigen tests are available in the marketplace as lateral flow immunoassay formats, requiring monoclonal antibodies as capture reagents, detection reagents, or both. This can be problematic as mutations occur. Immunoassays that detect the S protein are more susceptible to an increasing rate of falsenegatives and it is essential to obtain sufficiently accurate testing results to detect the virus during the pandemic.3
The Omicron mutations have also caused issues with potential therapeutics. Two monoclonal antibody therapies that inhibit the replication of SARS-CoV-2 were approved by the Food and Drug Administration (FDA) for Emergency Use Authorization (EUA). Early to the market, bamlanivimab combined with etesevimab from Eli Lilly, and casirivimab with imdevimab (RegenCoV) from Regeneron, proved to be effective treatments for mildto-moderate COVID-19 if given early enough at the onset of symptoms. The Omicron variant, with its novel mutations, has shown to be resistant to these therapies as evidenced by decreased drug efficacy. Subsequently, in January 2022, the FDA revoked their EUA, stating that ‘treatment agents are not expected to provide benefit to patients who have been infected with or exposed to the omicron variant.4
Benefits of pAbs in Infectious Disease Detection
Polyclonal antibodies can be a powerful alternative to monoclonal antibodies for diagnostic purposes. Isolated from hyper-immunized host sera, polyclonal antibody reagents are essential antibody pools from many different B-cells and may recognize many different epitopes on the target protein or antigen. ‘The ‘poly’ clonality of pAbs allows the binding of multiple antigenic determinants of the target. This allows pAbs to be more sensitive in certain assays against a variety of target proteins, cells or organisms… and are more likely to result in high-avidity binding, [with] the low likelihood of antigen ‘escape variants’ emerging.5
Indeed, the multiple epitopes on antigens available to pAbs are a powerful attribute. Independent studies have shown the ability of Rockland’s polyclonal to detect both the canonical SARSCoV-2 and the Omicron variant. Rockland has produced many antibodies to facilitate COVID-19 research and diagnostics, including both monoclonal and polyclonal antibodies to Spike and Nucleocapsid viral proteins of SARS-CoV-2. The image below shows the detection of the Omicron variant by immunofluorescence microscopy within infected A549 cells using polyclonal anti-Nucleocapsid antibody.
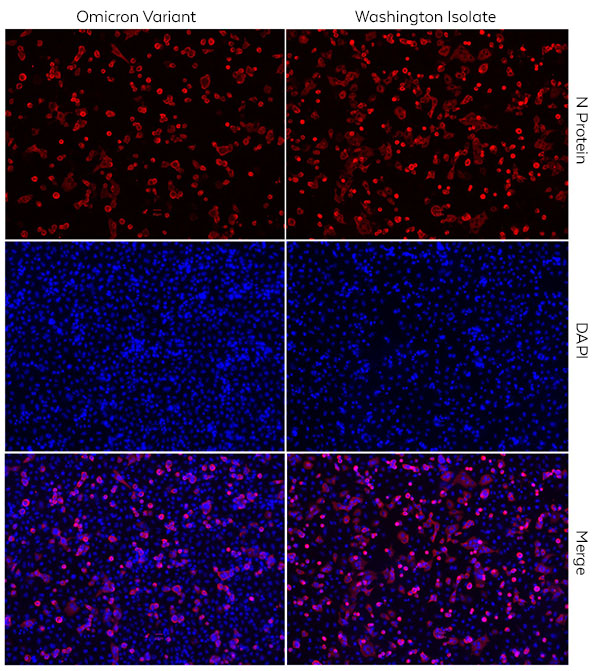
Figure: Immunofluorescence Microscopy. IF assay using Rabbit Anti-SARSCoV Nucleocapsid (N) Antibody, showing viral protein detection. A549 cells over-expressing ACE2 were either infected with the SARS-CoV-2 Washington isolate or Omicron Variant at an MOI of 0.5 for 24 hours. The cells were then fixed in 10% Formalin and stained overnight at 4ºC with primary antibodies directed against SARS-CoV Nucleocapsid (N) at 1:1000 dilution. Imaged using an anti-rabbit secondary conjugated to AlexaFluor 568 [red] and Nuclear Counterstain DAPI [blue]. Image Courtesy of Mohsan Saeed Lab/ Da-Yuan Chen, National Emerging Infectious Diseases Laboratories (NEIDL), Boston University
The Future of COVID-19 Research
Rockland has a long history of manufacturing high-quality polyclonal antibodies for the research and diagnostic markets. We currently provide both monoclonal and polyclonal antibodies specific to the Spike protein and Nucleocapsid (N) protein of SARS-CoV-2. While much can be said about the value of monoclonal antibodies, the versatility and robust nature of polyclonal antibodies cannot be overlooked. Intelligent antigen design and a manufacturing process that is constantly evaluated by the polyclonal antibody’s end use are crucial elements to good production and validation of antibodies. When produced and tested properly, polyclonal antibodies can have many long-term benefits.
Long after the pandemic has subsided, research will be conducted to further investigate various aspects of the virus, most likely including its origin, its relatively high mutation rate, and the variable rates of infectivity, transmissibility, hospitalization, and mortality that changed as different mutations became predominant on a global scale. Undoubtedly, highly specific antibodies, such as the monoclonal and polyclonal antibodies produced by Rockland against either the Spike protein or Nucleocapsid protein of SARS-CoV-2 will be critical tools for future research to be conducted into coronavirus biology. In addition to investigating the virus’s pathogenesis, understanding the cause of ‘long COVID’ and Multisystem Inflammatory Syndrome in Children (MIS-C) and how COVID-19 and MIS-C relate to toxic shock syndrome and Kawasaki disease, will likely also be the topic of research investigations globally.